
NEUROBOT >>
Workstation
NEUROBOT Workstation

The workstation is mechanically stabilized to prevent tipping and unintended movement during patient interaction. Its low center of gravity, weighted base, and medical-grade locking casters ensure secure positioning at the bedside. The enclosure and structural elements are built from durable, disinfectant-resistant materials that tolerate routine hospital cleaning protocols, including alcohol-based and hospital-grade antiseptic solutions. Surfaces are smooth and non-porous to support infection control standards.
NEUROBOT integrates a dual-screen therapeutic interface within a clinically optimized hardware architecture. The station supports supervised cognitive therapy, real-time monitoring, and structured rehabilitation workflows without compromising safety or regulatory considerations. Designed for continuous clinical use, it combines electrical reliability, mechanical stability, hygienic compatibility, and advanced therapeutic functionality in a single mobile platform suitable for modern hospital infrastructure.
Bedside therapeutic use
NEUROBOT Workstation is designed specifically for bedside deployment, allowing cognitive and neuro-rehabilitation therapy to begin early and continue consistently throughout inpatient care.
By bringing the therapy environment directly to the patient, the workstation eliminates transport barriers, reduces scheduling dependency, and enables therapy delivery even for patients with limited mobility, post-ICU conditions, or early-stage neurological impairment.
Bedside placement supports short, frequent, and structured therapy sessions — a critical factor in cognitive recovery and neuroplasticity — while maintaining a controlled clinical environment under professional supervision.
This model transforms the hospital bed from a passive recovery point into an active therapeutic setting, increasing both therapy accessibility and daily therapeutic volume without disrupting standard ward workflows.
Neurocub It is a multi-layered therapeutic system designed to continuously interact with the patient, analyze neurological responses in real time, and dynamically build an adaptive cognitive recovery pathway.
Neurocub Therapy Architecture & Patient Interaction Model.
The physical and digital environment where therapy happens. This includes the Neurobot station, the visual field, touch input, sound, voice interaction, and future extensions such as gaze tracking and emotional response recognition. This layer is responsible for delivering stimuli and capturing every form of patient response.
A structured therapeutic content engine consisting of cognitive cards, visual objects, sequences, recognition tasks, memory blocks, attention drills, and progressive exercises. This is not random content — each element belongs to a classified therapeutic category and difficulty spectrum.
The analytical core of Neurocub. Here, the system processes patient reactions: timing, accuracy, hesitation, repetition patterns, engagement drops, recovery signals, and response stability. Every interaction becomes a neurological data point.
This layer dynamically adjusts therapy parameters in real time: difficulty, pacing, repetition, sensory load, task complexity, and cognitive domain focus. Instead of static programs, each patient receives a continuously evolving therapeutic pathway.
Responsible for sustaining participation, emotional stability, and cognitive willingness. This includes positive reinforcement, progress signaling, micro-achievements, pacing control, fatigue management, and frustration detection. The goal is to keep therapy active without overwhelming neurological load.
The clinical interface layer. Here therapists and clinicians access structured recovery data: engagement trends, cognitive stability, response curves, improvement vectors, and regression alerts. This transforms therapy sessions into objective, trackable recovery dynamics.

Neurobot V.2.0
Supervised clinical workflow
NEUROBOT Workstation operates as part of a supervised clinical workflow, where all therapy activities are assigned, structured, and overseen by qualified medical or rehabilitation professionals.
Therapists define therapy programs, select exercises, and control session parameters remotely or locally, while patients interact with the workstation in a guided and standardized therapeutic environment.
The system enables clinicians to extend their therapeutic reach — supporting multiple bedside sessions across wards without the need for continuous one-to-one physical presence.
This workflow allows hospitals to scale therapy delivery, standardize cognitive rehabilitation protocols, and maintain clinical oversight while increasing the total volume of supervised therapeutic hours.

Therapeutic capacity & scalability
NEUROBOT Workstation is built to help hospitals increase daily therapeutic volume by making supervised cognitive therapy available at the bedside as a repeatable, deployable workflow.
Instead of relying on infrequent one-to-one sessions constrained by staffing and scheduling, the workstation enables short, structured sessions that can be delivered more consistently across more patients.
This approach expands clinical throughput: therapists can supervise and manage therapy programs across multiple rooms and units, while the workstation supports execution at the bedside within controlled parameters.
The result is scalable therapy delivery — more supervised therapeutic hours, better continuity of care, and a practical way to create new therapeutic capacity without proportionally increasing staff workload.
Example: Bedside Cognitive Exercise on Neurobot Station 1.3
This video demonstrates a real bedside cognitive exercise performed on the Neurocub Neurobot Station 1.3.
The workstation is positioned directly next to the patient’s bed, providing a stable and accessible interface for structured cognitive interaction without requiring patient mobility.
During the session, the patient engages with adaptive visual and cognitive tasks while the system continuously analyzes responses and updates the patient’s neurological profile in real time.
Such sessions are designed to be simple to initiate, comfortable to use, and suitable for daily repetition in post-acute, post-coma, or limited-mobility conditions.
The goal of the clinical deployment is to evaluate how Neurocub can transform passive bedside time into structured therapeutic engagement while reducing routine cognitive workload on clinical staff.
Neurocub Mini-Session >>
Core Interaction Algorithm.
I. Session Initialization
Before the first card appears, Neurocub forms a starting therapeutic context.
The system uses:
• history of previous sessions (if available)
• current cognitive profile of the patient
• therapist-defined parameters (if set)
• built-in safety baselines
Based on this, Neurocub determines:
• starting difficulty level
• allowed cognitive load range
• priority cognitive domains
• emotionally neutral themes
• session mode (activation, stabilization, development, support)
If the patient is new, the system launches in a safe baseline mode.
II. First Card Selection
The first card is not random.
It is selected:
• from the lowest difficulty range
• with a high probability of successful interaction
• with emotionally neutral content
• with simple, clear interaction mechanics
The goal of the first card is calibration, not training.
III. Patient Interaction Event
The patient interacts with the card.
Neurocub captures not only correctness, but the full behavioral pattern:
• reaction time
• response duration
• micro-corrections
• number of attempts
• returns and pauses
• voice activity
• emotional markers
• refusal or withdrawal patterns
Each card becomes a cognitive event, not just a task.
IV. Real-Time AI Analysis
After each interaction, Neurocub launches a real-time data analysis pipeline:
• raw behavioral signals
• interaction metrics
• cognitive indicators
• emotional markers
• fatigue signals
• overload risk patterns
• learning dynamics
From this, the system forms a momentary cognitive state — a live snapshot of the patient’s current neurological condition.
V. Dynamic Patient Profile Update
After each step, Neurocub updates a multidimensional patient model, including:
• attention stability
• processing speed
• error structure
• decision confidence
• learning gradient
• fatigue accumulation
• emotional feedback
• engagement continuity
The profile is not stored.
It evolves.
VI. Therapy Decision Layer
(Core intelligence point)
At this stage Neurocub does not choose a card.
It makes a therapeutic decision.
For example:
• continue the current domain
• shift the domain
• simplify
• increase complexity
• stabilize
• introduce a pause
• change interaction mechanics
• return to a comfort zone
• gently expand cognitive load
This is a clinical logic layer, not a content layer.
VII. Next Task Generation
Only after the therapeutic decision is made does Neurocub select the next card — based on:
• the updated patient profile
• the previous card
• session trajectory
• active therapy mode
• emotional response
• progression tempo
A card is chosen not because it is similar —
but because it is optimal for the patient at that moment.
VIII. Continuous Closed Loop
The cycle continues:
interaction → analysis → profile update → therapy decision → next task
until one of the following occurs:
• cognitive load limit is reached
• fatigue patterns emerge
• session objective is completed
• interaction quality declines
IX. Session Consolidation
At the end of the session Neurocub:
• consolidates global changes
• updates the long-term patient model
• generates a session snapshot
• flags clinically relevant events
• prepares structured data for the clinical dashboard
This transforms a session into a clinical unit, not just an activity.
What makes this system fundamentally different
• A card is not a picture. It is a measurement instrument.
• A response is not an answer. It is a neurocognitive process.
• A profile is not statistics. It is a living patient model.
• Card selection is not recommendation. It is a therapeutic decision.
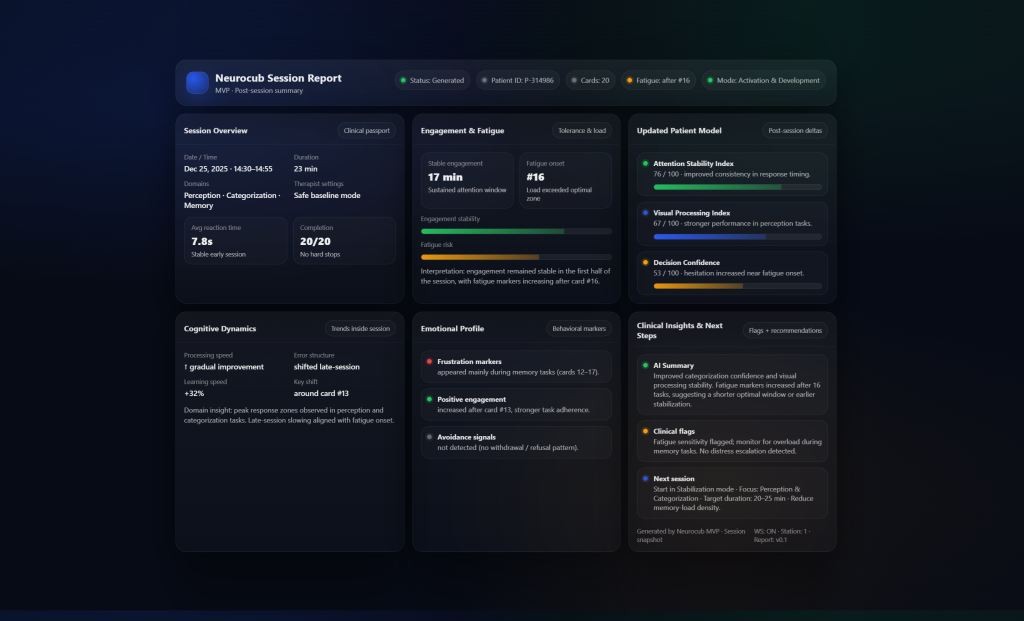
Neurocub Session Report — Core Blocks
This block provides the clinical passport of the session: duration, number of completed cards, therapy mode, and active cognitive domains. It defines the structural context of the session and serves as the reference frame for all further interpretation.
This section reflects how long and how stably the patient was able to interact with the system. It highlights engagement continuity, attention sustainability, and the moment when fatigue patterns began to emerge.
This block analyzes how cognitive performance evolved throughout the session. It reflects changes in processing speed, decision confidence, error structure, and learning patterns rather than isolated task results.
This section captures emotional and behavioral signals observed during interaction. It highlights frustration markers, positive engagement responses, motivation dynamics, and emotional stability throughout the session.
This block presents the updated multidimensional cognitive profile generated by Neurocub. It reflects changes in attention stability, learning speed, visual processing, fatigue sensitivity, and emotional response patterns.
This section summarizes clinically relevant events detected by the system and provides an AI-generated interpretation of the session. It highlights significant improvements, risk markers, and generates structured recommendations for the next session’s starting mode, load level, and cognitive focus.
Neurocub Session Report
Clinical Value & Clinical Deployment
Clinical Deployment. Building the future of cognitive recovery.
Neurocub is being introduced into real clinical environments as part of an early clinical deployment designed to explore a new model of cognitive recovery. The focus is bedside and in-room deployment, where patients can engage in structured cognitive interaction while the system continuously learns, adapts, and builds an evolving neurological profile. This stage is not about scale, but about clinical understanding — observing how adaptive cognitive systems can support rehabilitation workflows, enrich patient engagement, and generate new layers of recovery data.
By collaborating with hospitals, rehabilitation centers, and clinical teams, the Neurocub Clinical Deployment aims to validate therapeutic value, safety, usability, and clinical relevance. It is an exploration of how intelligent therapeutic systems can extend clinical capabilities, personalize cognitive recovery pathways, and transform passive hospital time into active neurological rehabilitation. This is the foundation of a future where cognitive recovery becomes measurable, adaptive, and continuously responsive to each individual patient.
Neurocub is designed as a scalable therapeutic system capable of supporting hundreds of patients in parallel across hospital departments and care environments. Every interaction generates structured data, allowing clinical teams to observe documented daily progress, emerging cognitive patterns, and long-term recovery dynamics instead of isolated session notes. As we see consistent, measurable cognitive engagement in patients, our goal is to extend this capability to as many individuals as possible who require daily neurological stimulation and structured recovery support. This clinical deployment marks the beginning of applying AI-driven analytics to cognitive therapy, forming the foundation for a new generation of adaptive, data-driven rehabilitation systems.
